Is Shockwave Therapy an Effective Treatment?
Shockwave therapy has become a popular option for people dealing with stubborn tendon, heel, and soft-tissue pain. But the big question is simple: does it actually work?
The answer is: it can be effective for certain conditions, especially chronic tendon-related pain, but it is not a magic cure or the right fit for everyone. The best results usually happen when shockwave therapy is used as part of a broader rehab plan that includes movement, strengthening, mobility work, and activity modification.
What Is Shockwave Therapy?
Shockwave therapy, also called extracorporeal shockwave therapy or ESWT, is a non-invasive treatment that uses acoustic pressure waves directed into painful or injured tissue. It is commonly used for conditions such as plantar fasciitis, Achilles tendinopathy, tennis elbow, patellar tendinopathy, and other chronic musculoskeletal problems.
The goal is not to “break up” tissue, as some people assume. Instead, shockwave therapy is thought to help stimulate a healing response, improve local blood flow, reduce pain sensitivity, and support tissue remodeling over time. NICE describes ESWT as a procedure that passes shockwaves through the skin to the affected area, with the aim of stimulating healing.
What Conditions Is It Most Often Used For?
Shockwave therapy is most commonly used for chronic conditions that have not improved with basic conservative care. These may include:
Plantar fasciitis: Heel pain caused by irritation or degeneration of the plantar fascia.
Achilles tendinopathy: Pain and stiffness in the Achilles tendon, often worse with running, jumping, or first steps in the morning.
Tennis elbow: Pain on the outside of the elbow related to tendon overload.
Patellar tendinopathy: Pain around the front of the knee, often seen in jumping or running athletes.
Rotator cuff or shoulder tendinopathy: Tendon-related shoulder pain, sometimes involving calcific deposits.
Research is strongest for some conditions and more mixed for others. Recent reviews suggest ESWT may improve pain and function across several tendinopathies, but studies vary in treatment protocols, energy levels, number of sessions, and patient selection.
So, Is It Effective?
For many patients, yes—shockwave therapy can be helpful, especially when pain has been present for months and standard treatments have not fully worked.
For plantar fasciitis, the evidence is generally supportive, although not perfectly consistent. A 2024 review of randomized controlled trials found ESWT has been studied as a treatment option for plantar fasciitis and included 14 studies with 867 participants. NICE states that ESWT for refractory plantar fasciitis raises no major safety concerns, but also notes that evidence on effectiveness has been inconsistent.
For Achilles tendinopathy, the evidence is more cautious. NICE reports no major safety concerns, but says the evidence for effectiveness is inconsistent and limited in quality and quantity.
For tennis elbow, the picture is also mixed. NICE states that ESWT for refractory tennis elbow raises no major safety concerns, but current evidence on efficacy is inconsistent.
In other words, shockwave therapy is not equally proven for every diagnosis. It appears most promising for chronic tendon and fascia problems, but outcomes depend on the condition, severity, treatment settings, clinician skill, and whether the patient follows an appropriate rehab program.
Why Shockwave Therapy May Work Better With Physical Therapy
Shockwave therapy may help calm pain and stimulate tissue healing, but it does not automatically fix the underlying movement, strength, or load-management issues that often contribute to chronic pain.
That is why it is often most effective when paired with physical therapy. A complete plan may include:
- Progressive strengthening
- Mobility and flexibility work
- Gait or movement assessment
- Balance and stability training
- Gradual return-to-activity planning
- Footwear, bracing, or orthotic guidance when appropriate
Think of shockwave therapy as a tool that may help restart or support the healing process. Physical therapy helps guide that healing in the right direction.
What Does Treatment Feel Like?
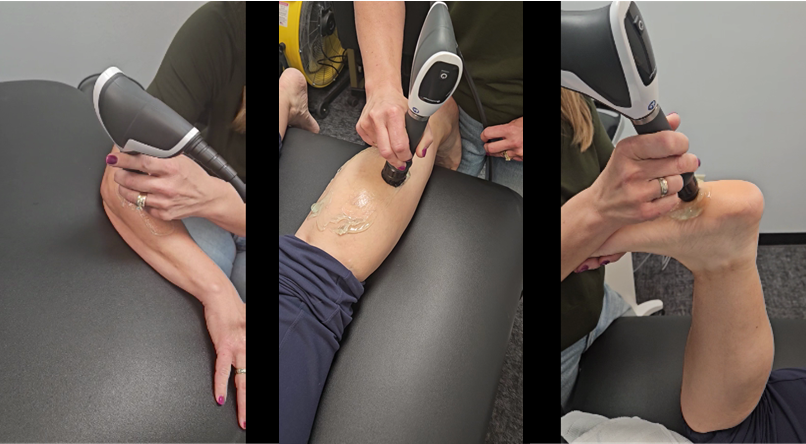
During treatment, a clinician applies a handheld device to the affected area. Patients often feel tapping, pulsing, or sharp pressure. The treatment may be uncomfortable, especially over sensitive tissue, but sessions are usually brief.
Some soreness afterward is common. Temporary redness, bruising, mild swelling, or pain at the treatment site can occur. Serious adverse events appear uncommon when ESWT is performed appropriately. A review noted that known side effects include pain during treatment and minor hematomas, with no severe complications expected when performed as recommended. Mayo Clinic also lists possible side effects such as skin redness, mild bruising, and pain at the application site.
Who Should Avoid Shockwave Therapy?
Shockwave therapy is not appropriate for every patient. It may not be recommended over areas involving pregnancy, certain tumors, severe infection, severe clotting problems, or specific sensitive tissues depending on the type and intensity of treatment. Mayo Clinic notes contraindications including a fetus or malignant tumor in the treatment area for low-energy radial and focused waves, and additional concerns for high-energy focused waves such as severe coagulopathy or treatment over lung tissue, brain, spine, epiphyseal plates, or malignant tumors.
Patients should always be screened by a qualified healthcare provider before beginning care, especially if they are pregnant, taking blood thinners, have a bleeding disorder, have cancer, have an active infection, or have significant nerve or vascular issues.
How Long Does It Take to See Results?
Shockwave therapy usually does not create instant healing. Some people feel improvement after one or two visits, while others notice progress gradually over several weeks. Chronic tendon and fascia problems often require time because the goal is tissue remodeling, not just temporary pain relief.
Many treatment plans involve a short series of sessions, often spaced about a week apart, though exact protocols vary widely. This variability is one reason research can be hard to compare across studies. A 2025 international expert consensus paper noted that ESWT may be an effective adjunctive treatment option in musculoskeletal injuries, but research is limited by major differences in treatment protocols.
Shockwave therapy can be an effective treatment for certain chronic musculoskeletal conditions, particularly tendon and fascia-related pain that has not responded to standard care. It is non-invasive, generally well tolerated, and may help reduce pain and improve function.
However, it is not a stand-alone cure. The best results typically come when shockwave therapy is combined with a personalized rehabilitation plan that addresses strength, mobility, movement patterns, and activity load.
For patients with stubborn heel pain, Achilles pain, elbow pain, or tendon-related injuries, shockwave therapy may be worth discussing with a physical therapist or qualified healthcare provider. The key is choosing the right patient, the right condition, and the right overall treatment plan. Our Total Sports Therapy Cave Creek location offers Shockwave Therapy. Visit our Shockwave Therapy Services page to learn more.